Documents obtained by NBC Bay Area’s Investigative Unit show medical staff at UCSF nearly quadrupled a young patient’s opioid medication and then failed to monitor him with a pulse oximeter, a simple medical device that would have alerted them if his blood oxygen level fell to a dangerously low level. The Patient Safety Movement, a non-profit group, estimates 250,000 patients die from preventable hospital errors each year.
As Melissa Pederson watched her son at UCSF hospital on a fall Saturday morning in 2015, it seemed like she and her family had successfully passed the most dangerous hurdle.
The previous day, doctors had removed a kidney from her son, Anders, and successfully transplanted it to her daughter, Kelly. A serious bacterial infection when Kelly was just 15 months old had compromised her kidneys.

Get a weekly recap of the latest San Francisco Bay Area housing news. Sign up for NBC Bay Area’s Housing Deconstructed newsletter.
“We really don't know where it came from,” said Melissa, “but she had total kidney failure. The doctors told me she had about a 30% chance to survive, but she was one tough little girl and she made it through.”
But just after Kelly’s 30th birthday, a blood test showed her kidneys were failing. Hearing the news, her younger brother Anders never missed a beat, and insisted on being the donor. He and Kelly had always been close.

During surgery there were no complications. Even though Anders was in severe pain, that was not unusual in kidney donors, and he managed to walk across the hall to his sister’s hospital room and tell her it was the happiest day of his life.
It was about 8:30 a.m. on the day after surgery when Anders asked his mother for his sunglasses. The sun was streaming in through the window, and he wanted to sleep after a rough night of vomiting repeatedly.
“I put the sunglasses on. I went down the hall and came back within probably three minutes,” said Melissa. “And he was really asleep. And I took the picture of him and I sat in his room.”
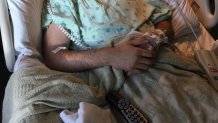
Her hope was that in a day or so, her kids might be released from the hospital. Kelly and Anders would hang out at the family home and recover together. "We bought matching pajamas to recover,” said Kelly, “and he bought a Chewbacca onesie to wear while we played video games that we could recover in. And we went to Costco and bought, you know, a bunch of food for my mom to make for us.
But as Melissa sat in Anders’ hospital room, something didn’t seem right. As a nurse worked on a computer behind Anders, Melissa approached her son. “I went over and I put my hand on his hand and his hand was cold, and then I took off his sunglasses and realized his face was yellow and his lips were blue - and I knew he wasn't breathing.” In the blur that followed, the nurse sounded the Code Blue alarm. Melissa remembers a group of doctors and nurses suddenly running into the room to revive her son.
“I actually had to leave the room because I thought it was going to throw up,” said Melissa.
Anders suffered a cardiac arrest. Melissa was told that perhaps he had a genetic heart defect. Doctors were able to restart his heart, but nine days later, it was clear that damage to Anders’ brain was extensive, and the family makes the tough decision to withdraw life support.
“When we were forced to pull the plug, when he went brain dead, his heart kept beating on and on and on,” said Kelly, “and I knew he didn't want to die. We were sitting there holding his hands and it's like you don't want to let go because you don't want it to actually be real."

“I think about him every day,” said Kelly.
“Twenty-four hours after he passed away I came home and I called UCSF, and I talked to the records department and I said I'd like my son's records, all my son's records,” said Melissa, “and they said, 'well, we don't have them available' …and I said, 'well, I would like you to make a copy and please have them available tomorrow.'" A month later, Melissa received a package in the mail, with 40 pages of documents.
“I was frustrated because it was impossible to have so few pages,” said Melissa. “He died in that hospital and we really wanted to know why.”

So, she hired Steve Hillyard, an experienced medical malpractice attorney. “I think there were forty-four thousand pages,” said Hillyard, after filing a lawsuit against UCSF and reviewing all the files. The paper trail documents the critical moments leading up to Anders’ cardiac arrest.
TIMELINE OF ANDERS PEDERSON AT UCSF HOSPITAL
For expert testimony, attorney Steve Hillyard turned to Doctor William Klein, who was professor of medicine at UC Irvine and had a decades long relationship with the University of California. “I have a great deal of respect for the facility,” said Dr. Klein. “Through the type of work that they do, they saved many lives, and they are a major research facility, as well as one of the top medical schools in this country.”

Doctor Klein testified UCSF made serious errors after Anders’ surgery. Anders wasn’t being monitored by a pulse oximeter, a simple device that would have alerted staff that his blood oxygen was dangerously low. What’s more, hospital records show when he stopped breathing, no one had checked his vital signs for nearly five hours. “Failure to do that every four hours is a breach of the standard of care,” said Dr. Klein
Another expert witness, Doctor Raffi Simonian, former director of the Department of Pharmacy at UC San Diego, testified he found at least 30 failures in Anders’ post-operative care.
Among those:
Hospital staff didn’t account for the effects of Dilaudid on someone who just lost a kidney. The drug’s packaging warns opioids should be given with caution and that initial doses should be reduced for a patient experiencing renal impairment.
...kidney function is diminished...until the kidney that's remaining is able to pick up the slack.
Deposition, Dr. Raffi Simonian, pg. 96,lines 11-13
From the pharmacist to the nursing staff, no one recognized the potency of the Dilaudid dose Anders was given.
...the floor nurses didn't recognize the potency issues. The nurse practitioner didn't recognize the potency issue. The pharmacist didn't recognize the potency issue.
Deposition, Dr. Raffi Simonian, pg. 134 line 24
Dr. Simonian testified Anders should have been watched carefully 24 hours after surgery, when the effect of the body’s natural adrenaline typically wears off.
...you can tolerate more pain medication sometime in that first 24 hours and not have respiratory depression...
Dr. Raffi Simonian Deposition, pg. 84 line 25
Simonian also testified that the Code Blue team failed to identify the cause of Anders Pederson's cardiac arrest. And, when Anders Pederson's heart stopped, Dr. Simonian noted that the medical team did not give him Narcan to reverse the effect of opioids.
“One mistake led to another, to another to another,” said Steve Hillyard. Mistakes, Hillyard believes, turned out to be fatal. “There's no doubt they killed him. It was preventable, it was foreseeable,” he said.
The San Francisco Superior Court agreed. After a traumatic trial the judge concluded the only reasonable explanation supported by evidence is that Anders died of an overdose of opioids, which was preventable.
...the Court is persuaded and concludes based upon the evidence presented that it is more likely than not that the Regents (of University of California) were negligent in administering Anders Pederson excessive opioids which caused him to suffer respiratory depression, resulting in cardiac arrest and brain death.
Court's Statement of Decision, Pg. 24 line 28
Despite that judgment, the University of California does not admit wrong-doing - citing two investigations that found “no fault on behalf of UCSF.” The hospital maintains Anders’ death “was not consistent with “excessive opioids.”
...the patient’s clinical course was not consistent with excessive opioids as the cause of death.
UCSF Statement to NBC Bay Area
However, UCSF did change its policy “after this incident” and now monitors transplant patients with “continuous pulse oximetry.”
But many hospitals still don’t do that. “Patients are getting harmed, and we have to do something to stop this and prevent this, and we can,” said Dr. Mike Ramsay, an anesthesiologist and CEO of the Patient Safety Movement, a non-profit with the goal of improving patient safety across the globe.

The organization has collected dozens of tragic stories about patients dying from medical errors. Based on statistical analysis, a study at Dartmouth Hitchcock Medical Center in New Hampshire estimates, conservatively, that 180,000 patients experience opioid-related adverse events, each year, often suffering effects such as brain or respiratory system damage.
According to the Patient Safety movement, 8,220 people die in hospitals every day in ways that could have been prevented. Many of the deaths and injuries, says Dr. Ramsay, could be prevented by using simple monitoring devices, like pulse oximeters.
“The solution is we need to monitor everybody. And really, your timeframe is not that great between when you stop breathing and when you're going to get hurt,” said Dr. Ramsay, adding, “and so we want the alarm system to be on the patient.
That may soon happen. The issue of opioid overdoses may soon be before congress. A new bill, the In-Patient Opioid Safety Act, would require all patients on opioids in hospitals to have continuous monitoring.
In the meantime, “Be an advocate for your loved one,” says Steve Hillyard. “Be an advocate for the patient who's not in a position to advocate for themselves.”
It’s a painful lesson the Pederson’s learned after Anders slipped away. “How could he not have a pulse oximeter on him, which I later found out is a doctor's choice to recommend to have the pulse oximeter,” said Melissa.
“My life will never be the same,” said Kelly. “My life is consumed by trauma from this, I hope no family ever has to go through this again.”
A San Francisco Superior Court ordered UCSF to pay the family two million dollars in damages, which was reduced to just $250,000. That’s because California law limits medical malpractice awards to $250,000. The Pederson’s maintain it was never about the money. They wanted answers, to help prevent it from happening to anyone else.

“We basically started our lawsuit just to get the records,” said Melissa Pederson. “We just wanted to know what happened, and since they weren't providing them, we felt we needed to get the records to figure it out. We wanted justice for him. He died in that hospital and we really wanted to know why.”

